Chronic Medication Management
 Chronic pain often starts after poorly healed trauma, failed surgery, or because of certain advanced diseases. When no other treatments can be offered to provide relief, medications may be necessary, alone or in conjunction with other interventions. Each patient’s case will be reviewed and appropriate treatment with Belbuca or opiates initiated for those that meet the criteria.
Chronic pain often starts after poorly healed trauma, failed surgery, or because of certain advanced diseases. When no other treatments can be offered to provide relief, medications may be necessary, alone or in conjunction with other interventions. Each patient’s case will be reviewed and appropriate treatment with Belbuca or opiates initiated for those that meet the criteria.
Belbuca is newly FDA approved Buprenorphine based medication for the treatment of chronic pain that was found to be effective in most conditions that require opiates. The advantages are lower side effect profile and diversion potential. You will need to be weaned off opiates to be switched to Belbuca and we offer an external device to help with withdrawal symptoms during the transition.
Opiates. Long-acting formulations could be prescribed to most compliant patients that meet criteria for chronic pain management and within the current daily limit of 90 MME or less. For patients who are currently on high daily dose opiate taper and usage of adjunct interventions will be offered as an alternative to switching to Belbuca.
Virginia Medical Marijuana Certificates
Blossom Pain Management & Green Medical has providers registered to evaluate a person’s condition and certify you for your Virginia Medical Marijuana Card. You are not required to be a patient in our pain management clinic for this evaluation. Please call our office for more details and visit norml.org for more information.
Chiropractic Manipulation
Coming soon/currently using large referral base.
Electrotherapy (TENS)
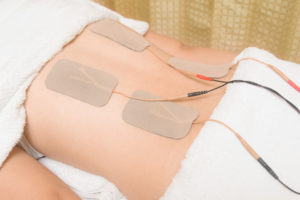 T.E.N.S. are used by hundreds of thousands of people all over the world for the relief of physical pain. TENS stands for (Transcutaneous Electrical Nerve Stimulation). which are predominately used for nerve related pain conditions (acute and chronic conditions). TENS machines work by sending stimulating pulses across the surface of the skin and along the nerve strands.
T.E.N.S. are used by hundreds of thousands of people all over the world for the relief of physical pain. TENS stands for (Transcutaneous Electrical Nerve Stimulation). which are predominately used for nerve related pain conditions (acute and chronic conditions). TENS machines work by sending stimulating pulses across the surface of the skin and along the nerve strands.
The stimulating pulses help prevent pain signals from reaching the brain. Tens also help stimulate your body to produce higher levels of its own natural painkillers, called “Endorphins”.
Tens units have different adjustable settings to control amplitude (intensity) of stimulation by controlling the voltage. Current, and pulse width (duration) of each pulse. Electrodes are placed at specific sites on a user’s body depending on the physical location of their pain. The current travels through electrodes and into the skin stimulating specific nerve pathways to produce a tingling or massaging sensation that reduces the perception of pain. When a Tens Unit is used as directed a T.E.N.S. is a safe, noninvasive, drug-free method for pain management. A Tens Unit is used to offer a better quality of life for people with pain. There are two ways to explain how a T.E.N.S. successfully decreases or eliminates pain.
One of these theories is called The Gate Control Theory and is the most advanced explanation. The gate-control theory suggests that there’s a neural mechanism in spinal cord that acts as a kind of gate, shutting down or opening the flow of signals from the periphery to the brain. Whether the gate is open, closed or partially closed depends on what sort of signal it receives from the brain to change the perception of pain in the user’s body. These frequencies interfere with the transmission of pain messages at the so spinal cord level and help block their transmission to the brain.
Another theory is called The Endorphin Release, which suggests that electrical impulses stimulate the production of endorphins and enkephalins in the body. These natural morphine-like substances block pain messages from reaching the brain, in a similar fashion to conventional drug therapy, but without the danger of dependence of other side effects.
Treatment for pain, anxiety, insomnia, and depression that’s proven to work
The Alpha-Stim electrotherapy device is proven effective and safe for pain management and treatment of anxiety, insomnia, and depression. It has no lasting side effects, no risk of addiction, and no danger of interaction with medications. Alpha-Stim helps you fight both the sleepless nights and the overwhelming sadness that can make it hard to get out of bed in the morning. It relieves both your nagging lower back pain and the constant burden of stress. Results are long lasting and often immediate.” We have a demo unit at Blossom for you to try.
Joint Injections
 Coming soon/currently using large referral base.
Coming soon/currently using large referral base.
Psychotherapy
Available through our extensive network of outside entities that will be chosen to compliment your comprehensive care plan for your pain.
Nutritional
Available through our extensive network of outside entities that will be chosen to compliment your comprehensive care plan for your pain.